Elder abuse
People living with dementia are vulnerable to abuse by people who are close to them, either in residential or home settings. They are also vulnerable to being taken advantage of by strangers because of their cognitive problems.
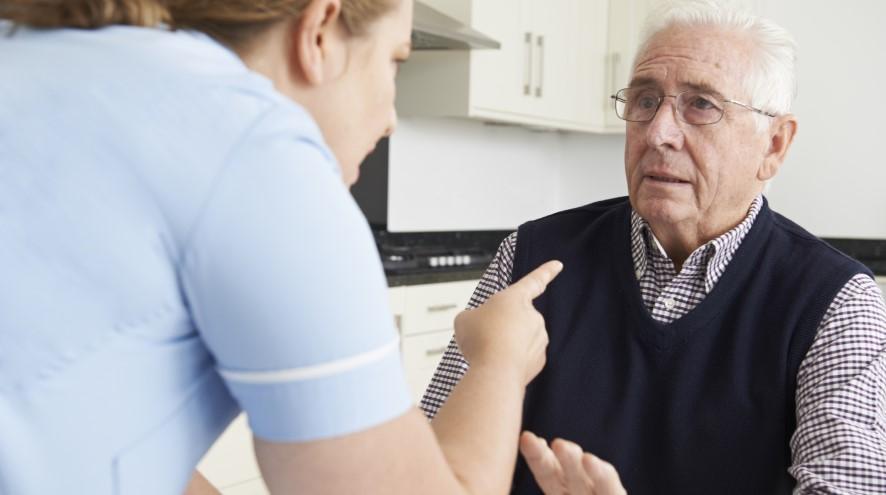
Overview
Abuse situations are often preventable through adequate support, training, supervision and legal protection.
Research has shown that abuse affects between 4% and 10% of older adults in Canada. Only one in five incidents of elder abuse comes to the attention of those who can help.
Abuse of older adults with dementia affects between 5.4% and 11.9%.
People with dementia are at increased risk of different forms of abuse (e.g. verbal, physical, financial and psychological abuse as well as neglect) due to their cognitive impairment, loss of capacity, communication challenges and increasing dependence on their caregivers.
The person with dementia may also abuse the caregiver or others either due to lifelong habits or impact of living with dementia.
The most common type of elder abuse
"Financial abuse is the most common form of elder abuse in Canada," says the Government of Canada's website. "Financial abuse can happen at any time, but it will often start after a health crisis or after the death of a spouse, partner or close friend. People who are alone, lonely or in poor health are more vulnerable."
At the same time, "Financial abuse can be difficult to identify or recognize. It is often a pattern rather than a single event, happening over a long period of time," says the Government of Canada's website.
The Government of Canada's information page for seniors about financial abuse defines it as "the illegal or unauthorized use of someone else's money or property. It includes pressuring someone for money or property."
For more tips, advice and action steps on this particular topic, visit the Government of Canada webpage "What every older Canadian should know about: Financial abuse."
Responding to a situation of abuse
In facilities and agencies
Facilities and agencies should have a protocol to deal with abuse. If you suspect abuse, take action immediately.
By caregivers
Providing care, which gets more onerous with the progression of dementia, can also be extremely stressful.
Risk factors for abuse by caregivers include:
- Lack of knowledge about dementia. Changes in behaviour, common among people with dementia, is particularly poorly understood, leading to stigma, blame and distress for caregivers2.
- High level of stress and inability to cope with it. Stress levels for dementia caregivers are five times greater than caring for a person with other conditions.
- Having no alternative strategies to address challenges that may come with living with dementia.
- Depression, which is common among caregivers.
- Lack of appropriate counselling and support.
- The caregiver’s perception that taking care of the elder is burdensome and without psychological reward.
By the person with dementia
Risk factors for abuse by the person living with dementia include:
- Intensity of a person’s illness or stage of dementia
- Change in mood and behaviour associated with dementia. Even people with no history of aggressive behaviour may become unintentionally abusive.
- The person’s own tendency toward verbal or physical aggression
Several risk factors affect both the person living with dementia and caregivers:
- The stress of care, mental and physical health problems can affect the coping abilities of both people with dementia and caregivers.
- Substance abuse
- Social isolation
- The person’s history of being abusive or having experienced abuse
- A history of domestic violence in the home
In many cases, elder abuse, mistreatment or neglect is unintentional.
Caregivers and people living with dementia pushed beyond their capabilities may not mean to be abusive, and caregivers may not mean to neglect the person in their care or ignore their needs.
Greater understanding of dementia and what to expect can be helpful. Making sure that caregivers have respite care breaks is also important. If, as a caregiver, you are having difficulty coping with stress related to caregiving, it is important to get the support you need, through a counsellor, faith-based leader, or someone through the Alzheimer Society.
More information and resources
- Canadian Centre for Elder Law
- Canadian Network for the Prevention of Elder Abuse
- Find family violence resources and services in your area - Government of Canada
- How you can identify abuse and help older adults at risk - Government of Canada
- Long-Term Care Task Force on Resident Care and Safety - An action plan to address abuse and neglect in long-term care homes
- National Initiative for the Care of the elderly (NICE) Assessment and Intervention Reference Guide - Note that this guide is no longer accessible online; the NICE website sells these guides in minimum orders of 20. However, a 10-page preview is available.
- Older Adult Abuse and Dementia - A Literature Review - Alzheimer Society of Canada
- Supporting Senior Victims of Crime - Online Training - MCIS
- What every older Canadian should know about: Financial abuse - Government of Canada
